Medical Model 3D Printing: Applications and Regulations
The rise of medical model 3D printing has fundamentally changed how surgeons prepare for complex operations and how patients understand their own anatomy. By converting 2D scans into tactile, high-fidelity physical replicas, medical professionals can now hold a patient’s heart or skull in their hands before making a single incision. This technology reduces operating room time, improves surgical precision, and serves as a vital tool for education and device validation.
What is Medical Model 3D Printing?
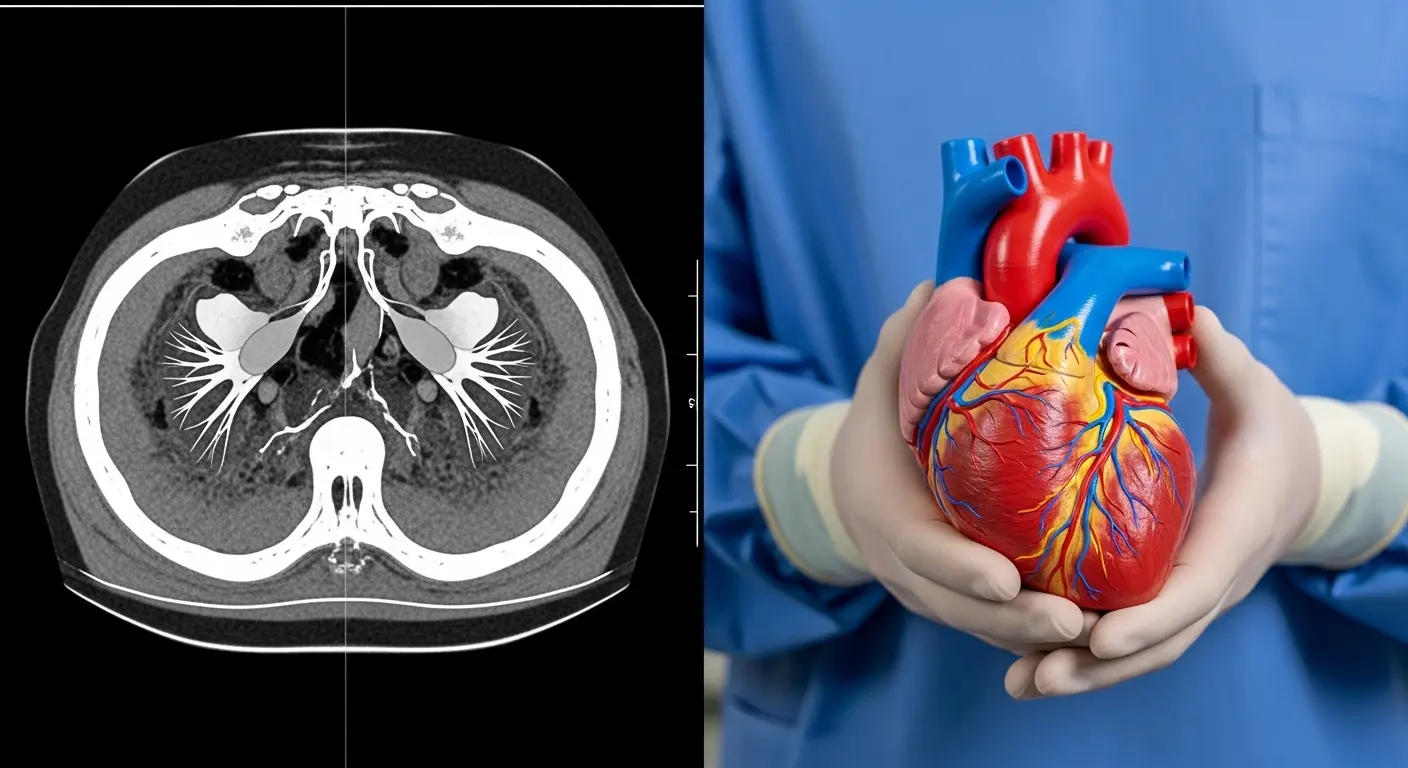
Medical model 3D printing is the process of creating anatomical replicas from patient-specific imaging data, such as CT or MRI scans, using additive manufacturing. These models serve as physical representations of organs, bones, or vascular structures, allowing for preoperative planning, surgical rehearsal, and the customization of medical devices and implants to a patient's unique geometry.
In my experience, the true value of these models isn't just in their "cool factor"—it’s in the data they provide. I remember a case involving a complex pediatric heart surgery where the 2D imaging was inconclusive about the vessel alignment. By utilizing 3D printing, the surgical team produced a multi-material model with clear vessels and a soft-tissue myocardium. They practiced the baffling procedure twice on the model, reducing the actual cross-clamp time in the OR by nearly 40 minutes. That is time that directly translates to better patient recovery.
How is 3D Printing Used in Modern Medicine?
Medical 3D printing is used for preoperative planning, creating patient-specific surgical guides, and developing anatomical models for medical education. It also plays a critical role in the rapid prototyping of new medical devices and instruments, allowing for functional testing and ergonomic refinement before moving into low-volume injection molding for clinical trials or final production.
The versatility of this technology is staggering. From dentistry to neurosurgery, the applications continue to expand as material science catches up with clinical needs.
| Application Category | Specific Use Case | Key Clinical Benefit |
| Surgical Planning | Complex bone fracture alignment | Reduced time under anesthesia |
| Patient Education | Explaining tumor pathology | Improved informed consent |
| Surgical Guides | Patient-specific drill templates | Higher accuracy in implant placement |
| Device Prototyping | Ergonomic testing of new scalpels | Faster R&D cycles |
| Prosthetics | Custom-fit limb sockets | Enhanced comfort and mobility |
Why is Preoperative Planning with 3D Models Growing?
Preoperative planning allows a surgeon to navigate a patient's unique anatomy in three dimensions. Using a physical model, they can pre-bend titanium plates or select the correct screw sizes before the patient is even on the table. This "rehearsal" phase is particularly vital in oncology, where understanding the exact spatial relationship between a tumor and major blood vessels can be the difference between a successful resection and a high-risk complication.
How Does 3D Printing Assist in Medical Device R&D?
For engineers, medical model 3D printing acts as the ultimate feedback loop. Instead of waiting for expensive tooling, they can use Top 10 Rapid Prototyping Manufacturers to create functional versions of a device. This allows for rigorous testing against anatomical models to ensure the device performs as intended in a simulated clinical environment.
What are the FDA Regulations for Medical 3D Printing?
The FDA regulates medical 3D printing by classifying devices based on risk and requiring strict "Quality System" (QS) regulations for manufacturing. While anatomical models used for education are generally low-risk, 3D printed surgical guides and patient-specific implants must undergo rigorous validation, documentation of the digital-to-physical workflow, and material biocompatibility testing to ensure patient safety and device efficacy.
Navigating the regulatory landscape is often the hardest part of medical innovation. The FDA’s "Technical Considerations for Additive Manufactured Medical Devices" guidance document provides a framework, but the burden of proof lies with the manufacturer.
Understanding Class I, II, and III Classifications
Most 3D printed anatomical models used for planning fall under Class I (low risk). However, if that model is used as a diagnostic tool, it may move into Class II. Surgical guides are typically Class II, requiring a 510(k) submission. Patient-specific permanent implants are the most regulated (Class III) and require the highest level of clinical data.
The Importance of Software Validation
In medical printing, the software is just as important as the printer. You must use FDA-cleared software for "segmenting" the CT/MRI data into a 3D file. If the software inaccurately interprets the scan data, the physical model will be flawed. This is why many hospitals partner with Top 20 Rapid Prototyping Manufacturers who maintain ISO 13485 certification for medical device quality management.
Which Materials are Best for Medical Anatomical Models?
The best materials for medical anatomical models include clear photopolymers (SLA) for visualizing internal structures, rigid resins for bone simulation, and soft elastomers for mimicking cardiovascular tissue. For functional prototypes and surgical guides, biocompatible materials like Nylon (PA12) or medical-grade Titanium are used because they can withstand sterilization processes and safely contact human tissue or fluids.
Simulating Bone and Soft Tissue
When we build a model for an orthopedic surgeon, we use materials with a specific shore hardness to mimic cortical and cancellous bone. For a cardiologist, we might use a PolyJet material that allows for varying levels of flexibility. This enables the surgeon to actually "suture" the model or feel the resistance of a valve—a level of realism that was impossible a decade ago.
| Material Type | Medical Application | Key Property |
| SLA Resins | Clear surgical guides, clear organs | High transparency and detail |
| Nylon (SLS) | Functional instruments, bone models | High strength and heat resistance |
| Titanium (DMLS) | Permanent implants, plates | Biocompatible and osseoconductive |
| TPU / TPE | Vascular models, heart replicas | Flexible and tear-resistant |
Dealing with Sterilization and Biocompatibility
If a 3D printed part is going into the sterile field of an OR, it must be capable of surviving an autoclave or ethylene oxide (EtO) sterilization. Many standard 3D printing resins will warp or become brittle under these conditions.
Tip: When selecting a material for a surgical guide, always check the USP Class VI or ISO 10993 rating. These certifications prove the material won't leach toxic chemicals when in contact with the body.
How Does 3D Printing Compare to Traditional Medical Manufacturing?
3D printing offers superior geometric freedom and speed for patient-specific parts, whereas traditional manufacturing like injection molding is better for high-volume, standardized components. In the debate of molding vs. 3d printing, 3D printing is the clear winner for the "Quantity of One" (individual patients), while molding remains the gold standard for mass-market medical disposables.
The Cost of Customization
The cost of a custom-machined implant could be $10,000, while a 3D printed equivalent might cost $1,000. This price drop has democratized access to personalized medicine. However, once you need 50,000 units of a standard syringe or connector, the cycle time of a printer cannot compete with the 10-second cycle of an injection mold.
How to Implement 3D Printing in a Clinical Setting?

Implementing 3D printing in a clinical setting requires a workflow that includes data acquisition (CT/MRI), image segmentation, 3D printing, and post-processing. This "Point-of-Care" (POC) manufacturing must be overseen by a multidisciplinary team of radiologists, surgeons, and engineers to ensure the physical model accurately reflects the clinical reality and meets all hospital safety standards.
The Digital Workflow Steps
- Imaging: High-resolution CT or MRI scans are taken of the patient.
- Segmentation: Software is used to "mask" or isolate the specific anatomy (e.g., the liver) from the rest of the scan.
- Refinement: The 3D file is cleaned of noise and artifacts to ensure a smooth print.
- Printing: The file is sent to a validated 3D printer using the appropriate medical-grade material.
- Post-Processing: The model is cleaned of support structures, cured (if resin), and sterilized if necessary.
Challenges of In-Hospital Printing
The biggest challenge isn't the hardware; it's the liability. Who is responsible if a 3D printed guide fails? This is why many institutions prefer a "Hybrid Model," where the design is done in-house, but the actual printing is outsourced to specialized 3d printing bureaus that carry the necessary insurance and certifications.
What are the Limitations of Medical 3D Printing?
The limitations of medical 3D printing include the high cost of medical-grade materials, the time required for image segmentation, and the current inability to print fully functional, vascularized living organs. While "bioprinting" is a growing field, we are still years away from printing a replacement kidney that can be successfully transplanted into a human patient.
Surface Finish and Resolution
While high-end printers offer incredible detail, the "stair-stepping" effect of layers can still be an issue for extremely fine vascular structures. If a model needs to be perfectly smooth for fluid flow studies, extensive manual post-processing is required, which adds time and cost to the project.
Data Privacy and Security
Because every 3D printed medical model is based on a patient's personal scan, data security is paramount. DICOM files contain sensitive HIPAA-protected information. Manufacturers and hospitals must ensure that the digital thread is encrypted and that no patient-identifiable data is left on the printer’s local storage.
Future Trends: AI and Bio-Fabrication
The next decade of medical model 3D printing will be driven by Artificial Intelligence. AI algorithms are already beginning to automate the tedious "segmentation" process, turning hours of manual work into a few minutes of automated processing. This will make 3D printed models a standard part of every complex surgery, rather than a luxury reserved for specialized cases.
Furthermore, we are moving toward "4D Printing," where parts can change shape or function in response to heat or moisture once implanted. This could lead to stents that expand precisely as a child grows, reducing the need for repeat surgeries.
Designing for Medical Precision (DfAM)
To get the most out of an anatomical model, designers must follow specific Additive Manufacturing (AM) rules:
- Hollow Structures: To save material and cost, large bone models should be hollowed out with internal lattices for strength.
- Escape Holes: If you are printing a hollow heart, you must include holes to allow uncured resin or powder to escape.
- Orientation: Print surgical guides in an orientation that minimizes supports on the "mating surface" that touches the bone to ensure a perfect fit.
Final Thought
The evolution of medical model 3D printing is a testament to the power of merging digital data with physical craftsmanship. As regulations become more standardized and materials more sophisticated, the barrier to entry for personalized surgical planning continues to fall. For the modern surgeon, these models are no longer optional "extras"—they are essential maps for navigating the most difficult terrains of the human body. By embracing these tools, the medical community isn't just innovating; it's fundamentally improving the safety and success of patient care worldwide.

